Compressed air systems are often an afterthought in health care. Equipment requiring compressed air is often limited and areas needing it are usually localized. Moreover, compressed air is not a life safety system like medical air is; therefore, it is not held to the same quality standards. Still, compressed air is needed in almost all health-care projects where surgery and sterile processing occur — it is a necessary system for both.
Instrument Air Vs. Service Compressed Air
Beyond medical compressed air, a topic too lengthy to discuss here, the two air system types most often encountered in health care are instrument air and service compressed air. Like medical air, instrument air is a medical gas and subject to the requirements of NFPA 99 Chapter 5.
Instrument air is defined as a medical support gas under NFPA 99 and required to be delivered at pressures, cleanliness or purities specific to its intended function. These criteria are almost always determined by the equipment it is connected to, such as surgical tools, instrument dryers, boom brakes and others.
ISO Standard 8573-1 is one of the most used standards that classifies compressed air into varying levels of quality (i.e., purity and cleanliness), and most medical equipment will require a quality falling into one of the classes the standard defines. ISO 8573-1 lists criteria for solid particulates, water and dewpoint, and oil for each class, as shown in Table 1.
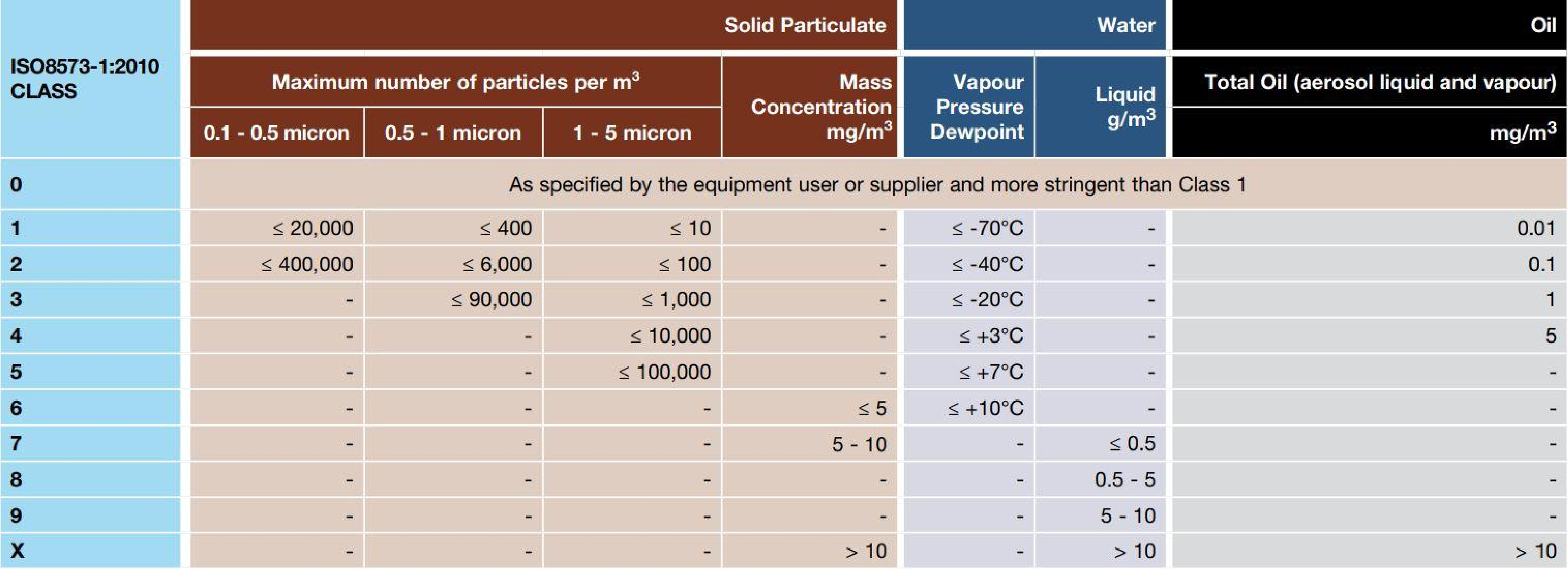
It should be noted that Class 0 (the most stringent) does not list specific values for these criteria but instead leaves them to be specified by the equipment or user. Therefore, equipment calling for Class 0 air has ambiguous requirements unless it also specifies particulate sizes, dewpoint and oil concentration.
Beyond pressures and quality, NFPA 99 also has requirements for instrument air generation and monitoring, similar to other medical gases. Instrument air may be generated by either high-pressure cylinder manifolds or by air compressor plants, but each is subject to NFPA 99 redundancies.
Manifolds must have reserve headers, and plants must have a redundant compressor. Additionally, the source equipment must be monitored by a local alarm and two master alarms in continuously staffed areas of the building.
Service compressed air, like instrument air, has delivery pressure and quality requirements driven by the equipment the system is connected to. This equipment can include pneumatic tools in maintenance shops, air guns in sterile processing areas, pneumatic door openers on washers and sterilizers, and others. However, service compressed air is not held to the generation and monitoring standards of NFPA 99; instead, it is left to best design practices based on the engineer’s intuition and user preferences.
When choosing whether a system should be classified as instrument or service compressed air, consider the connected equipment. If failure of the system could impede the function of the equipment and, in turn, impede a surgical procedure in progress, then the system should be classified as instrument air. For example, compressed air connected to equipment booms and pneumatic surgical tools should be classified as instrument air.
Other equipment where failure would not impede a surgical procedure in progress may be able to be defined as service compressed air. For example, compressed air connected to a washer disinfector in a sterile processing area could be classified as service compressed air.
Common Connected Equipment
The three areas in a health-care building most likely to require compressed air are surgical suites, sterile processing areas and maintenance shops/biomedical work rooms.
Surgical suites typically need compressed air to drive tools and for pneumatic brakes in equipment booms (see Figure 1). Connections for surgical tools may be contained in air outlets in the walls or ceilings or directly on equipment booms. Connections to pneumatic boom brakes are made at the base of the boom in the ceiling.
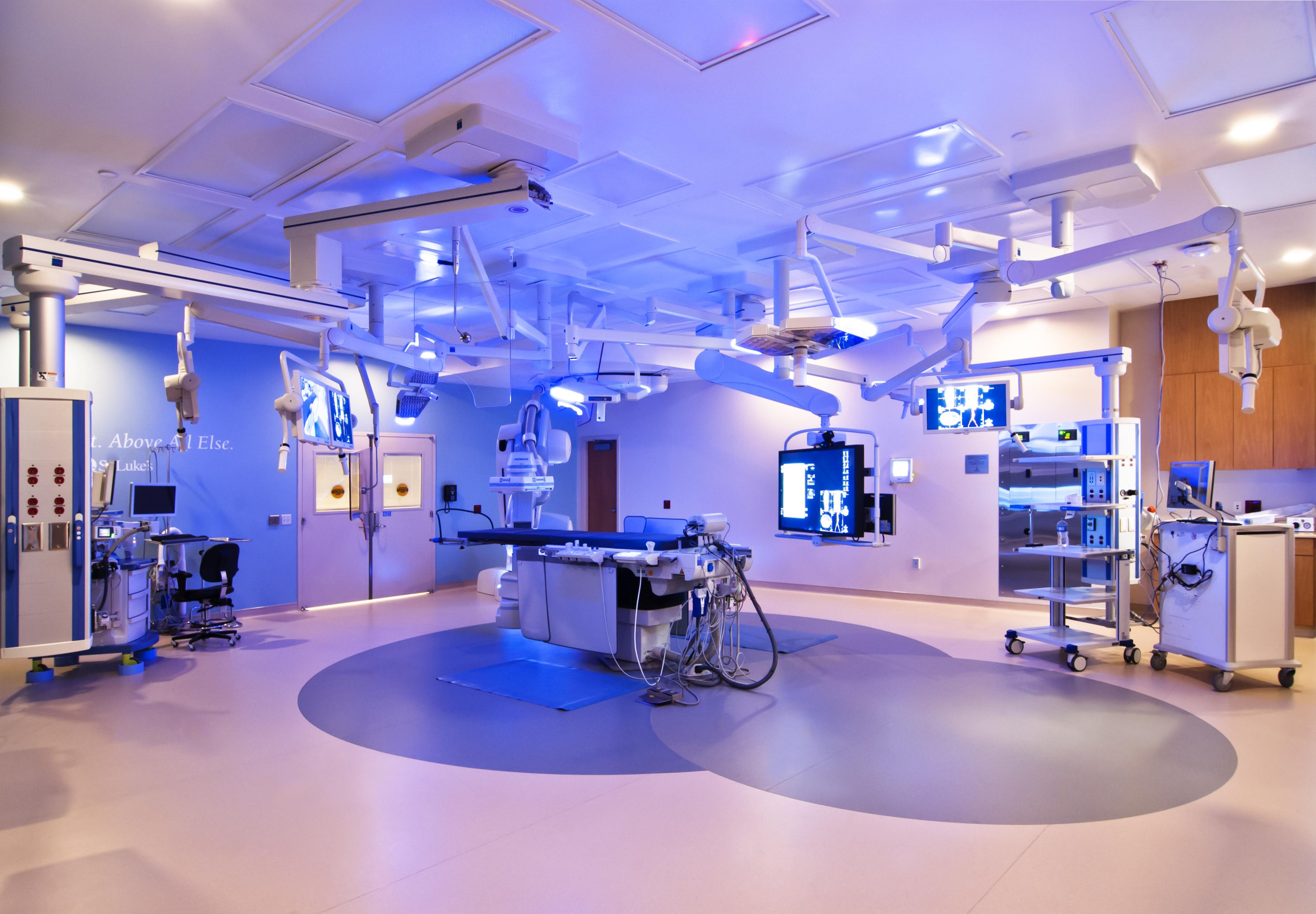
Sterile processing areas often require compressed air for pneumatic door openers on washers and sterilizers, air guns used for instrument blowdown and dedicated instrument drying units. Many of these connections are handled through wall or ceiling outlets with flexible hose connections to the equipment.
Maintenance shops may be stocked with an array of pneumatic work tools for bed and cart repair and the like. Users will usually ask for compressed air wall outlets so they can connect flexible hoses to the tools.
General Design Considerations
• Source equipment. Determining the compressed air source equipment is usually the first step in designing the system (see Figure 2). High-pressure manifolds usually only make sense in small facilities with small systems and where the first cost of the project does not allow for air compressors. However, when accounting for costs of air cylinder deliveries, compressors are almost always less expensive over the life of the building.

When considering air compressors, determine the redundancy requirement first. If classifying the system as instrument air, NFPA 99 requires a redundant compressor. However, even if the system can be classified as service compressed air, a redundant compressor may still be a good idea.
For example, if failure of the compressor could halt surgical instrument sterilization in a hospital with a heavy caseload of emergency surgeries, a redundant unit would be critical. The piping diagram (Figure 3) shows a duplex source equipment setup with redundancies appropriate for a case like this.
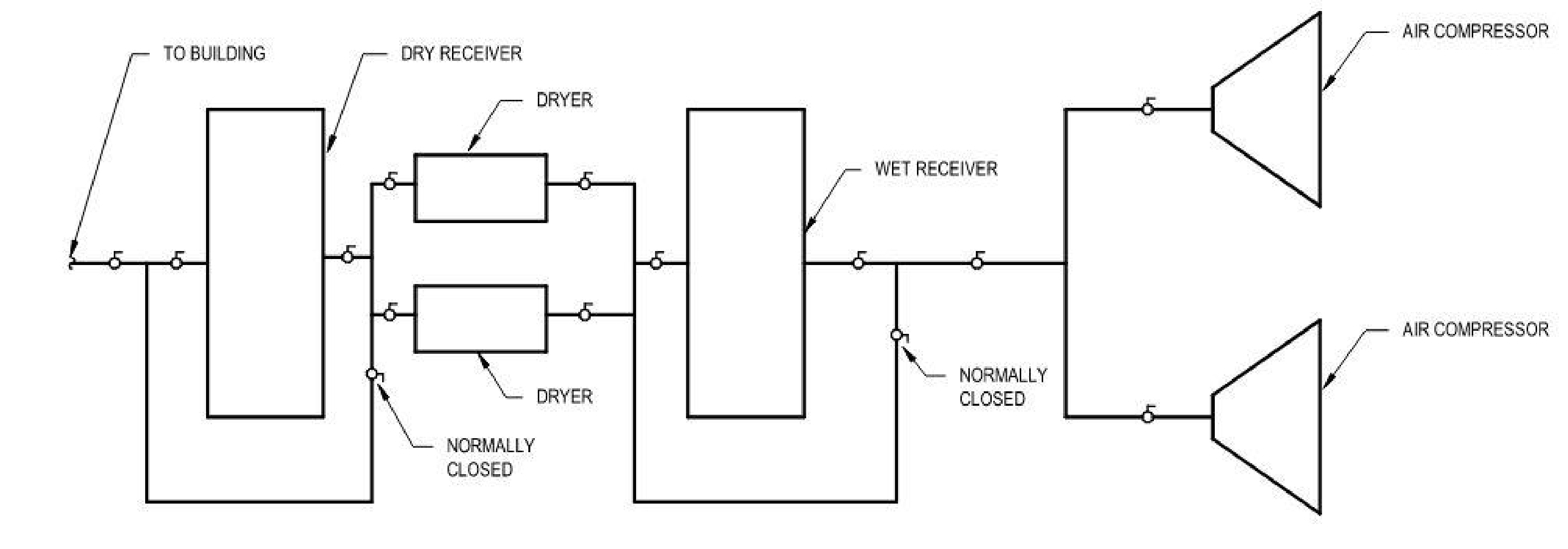
As the piping diagram shows, compressors are only one component of the source equipment. Air dryers are also necessary to keep the pipeline free of condensate, which can promote the growth of biological contaminants. Redundant dryers that run constantly are the best insurance to keep condensate out of the pipeline.
If you must use only one dryer, make sure the air compressor will automatically shut down if the dryer fails; otherwise, you run the risk of condensate in the pipeline. Dryers will use either a refrigerator, permeable membrane or solid desiccant to dry the air; which you choose is often driven by the air dewpoint requirement.
Refrigerated dryers can generally handle all ranges of airflow capacities but tend to be limited to a dewpoint of
3 C (37.4 F). Most membrane dryers can handle dewpoints down to -40 C (-40 F) and sometimes further, but they are limited to airflows of around 100 cubic feet/minute. Desiccant dryers are often the best choice for systems requiring very low dewpoints and high airflows, as they can handle down to -100 C (-148 F) and all ranges of capacities.
In addition to compressors and dryers, air receiver tanks are another major element of source equipment. Receivers are essential to optimize the system and prolong the life of more costly components. Wet receivers allow moisture, oil and particulates to precipitate out of the air before going to the filters on the dryers, prolonging the life of both.
Dry receivers keep the compressors and dryers from short cycling or becoming overtaxed. They provide a limited supply of stored compressed air that can be delivered to the equipment without triggering the source equipment and provide a buffer in times of high demand.
• Pipeline. Selection of pipeline materials, joining methods and accessories also is essential to an optimal system. Schedule 40 black steel piping with threaded or welded joints is often the most economical choice, but it is susceptible to oil and rust contamination and, therefore, not the best option. Schedule 10 or 40 stainless steel with flanged or welded joints is on the other end of the cost spectrum but usually only needed in corrosive environments.
Type L copper is the most common pipe material as it is competitive in terms of cost, cleanliness and durability. Some designers prefer heavier-walled Type K copper for pressures in excess of 200 pounds/square inch.
Joining methods include soldering or brazing, the latter offering a lower risk of contaminants in the pipe if a dry nitrogen purge is used during joining. Brazing is, therefore, a better option when very clean air is needed, such as when it will be used to dry surgical instruments.
Drawings for compressed air systems and pipelines generally follow the same rules as other plumbing systems. If you are dealing with an instrument air system, it should go on your medical gas drawings, as it will be subject to the requirements of NFPA 99 and reviewed under those rules.
When dealing with a service compressed air system, put everything on the normal plumbing drawings; if you put this system in with other medical gases, code reviewers and verifiers will expect the system to meet the more restrictive NFPA 99 requirements.
Many manufacturers offer packaged compressed air source equipment that may work well for small systems. These packaged systems provide all the compressors, receivers, filters and monitors to deliver either instrument or service compressed air to the building.
However, as with most other health-care plumbing systems, it is up to the designer to understand the nature and importance of the connected equipment, the implications of system maintenance or failure and other user expectations. Discussing these with a manufacturer before selecting equipment helps ensure the facility will get the most ideal system for its needs.
Aaron Bock, PE, is a senior plumbing engineer at ERDMAN, a provider of health-care and senior living strategy and design. He has been designing plumbing systems for these markets for more than 15 years. Bock is a past president of the American Society of Plumbing Engineers’ Wisconsin chapter, an advocate of integrated design, and a graduate of the College of Engineering at UW-Madison.


_800x800_webp.webp?t=1775667064)



