Emergency departments are a fast-growing health-care market in the United States. Freestanding emergency departments (those housed in their own building separate from a hospital) are seeing increased demand as health-care cost pressure shifts care from inpatient, hospital-based care to less expensive outpatient sites (https://bit.ly/3AIFMls). They are required by code to have facilities that serve several functions, and one of these is a decontamination area (see Figure 1).
Health-care professionals use these areas to wash and decontaminate patients that have been or may have been exposed to hazardous substances and to contain the substances until they can be disposed of. Plumbing systems for these areas must be designed with this in mind while serving the equipment used for treatment.

What the Codes Say
Before undertaking the design of an emergency decontamination area, it is important to know what codes govern the design and what they say. Health department regulations, building codes and plumbing codes may each direct the design of these plumbing systems.
• Facility Guidelines Institute. Most U.S. state health departments have adopted some version of the Facility Guidelines Institute’s (FGI) guidelines for emergency departments (an interactive map of these states can be found at https://bit.ly/3rcSPZ2). States that have not adopted them often have similar language in their building codes or health department regulations; having familiarity with the FGI guidelines is still useful for projects in these states.
The FGI guidelines have multidiscipline requirements for emergency decontamination areas, but those important to plumbing are the following (https://bit.ly/3IQRNbf):
1. Two shower stations with hand-held wands and temperature controls must be provided, along with a floor drain. Water discharge from the showers must be contained inside the room, which usually means sloping the floor away from the perimeter toward the floor drains and equipping the doors with saddle thresholds.
2. Shower and other plumbing fixtures in the room must be acid-resistant, as aggressive chemicals are used to clean the room after use.
3. A dedicated holding tank for the shower waste must be provided to keep hazardous substances out of the public sewer if required by the local authority having jurisdiction.
4. Portable or hard-piped oxygen and portable suction must be provided; most clients prefer portable services.
• Plumbing codes. These codes are largely silent on the design of emergency decontamination areas and, instead, defer to health department regulations or building codes. However, most plumbing codes require an interceptor anywhere that substances harmful to the public sewer could be introduced.
In this case, the interceptor is the holding tank for the shower waste mentioned previously. Beyond providing the holding tank, plumbing codes require that they be installed and maintained per the manufacturer’s
recommendations.
Early Design Considerations
Code language rarely provides all the direction needed to design an emergency decontamination area according to a client’s needs. There are many other considerations that need to be accounted for outside of code requirements, which may be driven by the project type, location, client or good design practices.
• Project location, type and likely hazards. An emergency decontamination area should be equipped for the types of cases that it is most likely to see. The most common case types are driven largely by the building’s location and size. For example, a small emergency department in a rural area usually sees very different types and frequencies of cases than a large one in a densely populated city. The former type is more likely to see accidents involving petrochemicals, fertilizers, pesticides and methamphetamine manufacture.
Emergency departments in suburban and urban settings still see a fair amount of petrochemical exposure but are also more likely to deal with toxic industrial chemicals, radiological agents and harmful construction dust, including asbestos.
• Likelihood of mass casualties. Consider the likelihood of a nearby mass casualty event when designing these areas. Emergency departments in densely populated areas are the most likely to deal with these events, but those in more rural areas are not exempt from them.
Emergency departments in urban settings tend to see mass casualty events involving transportation and manufacturing but may also want to be prepared for terrorist attacks involving chemical, biological or radiological agents.
When choosing fixture types and quantities for those in more rural areas, you should consider their proximity to potential hazards such as rail lines that carry chemical tankers, power plants, petrochemical pipelines, and manufacturing facilities. Also ask your client how many cases they want to be able to process per hour.
• Auxiliary/modular decontamination areas. While mass casualty events are an important factor to consider when designing emergency decontamination areas, many health-care systems are cautious in how much permanent space and infrastructure they are willing to devote to them. Instead, they often opt for modular or mobile decontamination units that can be quickly deployed when needed for a large influx of cases (see Figures 2 and 3).

These units come with a wide variety of construction and MEP system options — some units are simple tent structures with effluent containment curbs that must be manually drained and supplied with outside water and showers, while others are mobile trailers that have self-contained water supplies and heaters, showers and waste-holding tanks.
When dealing with modular units, it is important to understand their requirements and the client’s strategy for deploying them from the onset.
Design Elements
Once you have answers to your early design phase questions, many of the major plumbing components can be chosen.
• Shower number and type. As discussed, most codes require that a decontamination area must have no fewer than two shower stations, and each must have hand-held wands and temperature controls. The codes, however, do not give any requirements on shower flow rates, leaving this decision to the engineer and the client.
For small emergency departments that have infrequently used decontamination areas, clients may be satisfied with standard 2.5 gallons/minute (gpm) showers. Larger facilities with higher caseloads typically demand these along with fixed overhead drench showers that discharge at 20 to 30 gpm. It is important to determine which of these your client is expecting early on, as it drives the rest of the systems that serve the area.
Additionally, shower controls should be set to deliver water at no more than 100 F and at a pressure that will aid decontamination without causing injury (50 to 70 pounds/square inch (psi) is common).
Two shower stations are often not enough to keep up with the caseload the client wants capability for. When determining the number of showers, consider the number of cases the client wants to process per hour, along with a shower time of no less than 15 minutes per patient.
• Shower accessories and other fixtures. Many clients want other supplementary fixtures to handle the types of cases they anticipate. Showerheads and wands are useful for patients that are conscious and mobile, but patients arriving incapacitated and on gurneys are not uncommon.
In these cases, it may be easier for health-care professionals to use spray heads on retractable hoses to decontaminate patients. These hose stations can be placed either overhead or on the walls according to client preference, should be equipped with easily accessible thermostatic temperature controls, and be regulated to the same pressures as the showers.
Equipping them with robust anchorage is also a good idea since the spray heads may get caught on passing gurneys during heavy caseloads — work with your structural engineer to determine the best method.
Showers and spray heads are useful for washing down patients’ bodies and extremities, but they are not appropriate for washing the eyes and face as their water volume and pressure may cause injury. Dedicated eye and face wash fixtures conforming to ANSI Z358.1 should be provided for these instances (https://bit.ly/3gaQ18M).
• Decontamination tank and controls. Once the number and types of fixtures have been determined, the waste-holding tank can be designed. Clients tend to be most interested in its size and controls, but its location is important as well.
At a minimum, the tank should be sized to hold the total discharge from all decontamination fixtures if they were to run simultaneously for 15 minutes. However, many clients want far more capacity than this, especially if they want to be prepared for mass casualty events.
If this is the case, determine the total number of cases the client wants to be able to process in a given event, and then assume each case requires a 15-minute washdown from the fixture with the highest flow rate. Drainage pipe should be likewise sized to handle maximum flow from all fixtures at once.
How the holding tank interfaces with the primary building waste system is also subjective by the client. Fixture waste may be routed directly to the tank, where it must later be removed by a hazardous materials (hazmat) pump truck. However, the waste is not always hazardous to the building sewer, such as when the decontamination area is washed down and cleaned.
Calling a pump truck to empty the tank in these instances can become costly and time-consuming, so many clients prefer to have the means to divert the waste to either the holding tank or the building waste system. This usually means putting a diverter valve upstream of the holding tank that allows the staff to choose where the waste goes, as shown in Figure 4.
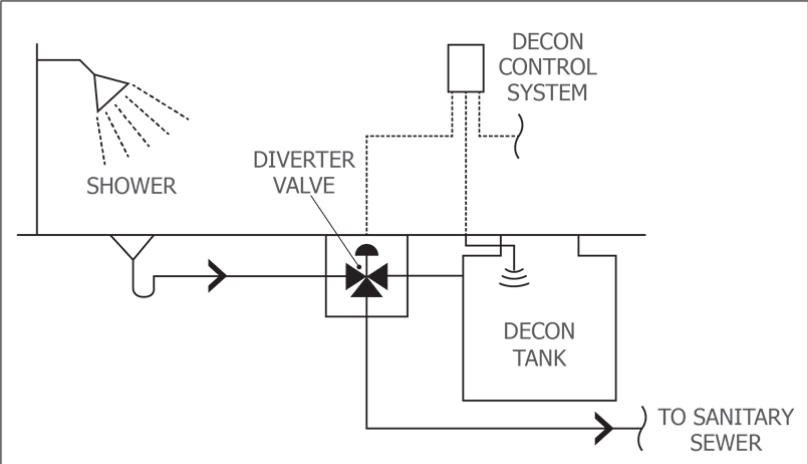
Less commonly, clients also want a valve on the outlet of the tank so that it can be opened and drained to the building sewer if the waste is nonhazardous. Post-indicator-type valves can be used in both cases, but electrically actuated valves with control panels are often a better choice since they can be activated more quickly in emergencies.
These valves should be placed in watertight valve boxes below the floor for maintenance access. Their corresponding control panels should be placed where they are readily visible and accessible — immediately outside the patient entrance to the decontamination area is common.
In addition to control valves, many engineers equip decontamination tanks with sensors and alarms that alert staff when the tank is getting full. Connecting the alarm to the building monitoring system is also a good idea. Finally, tanks should also be equipped with a sampling port so that hazmat staff can remove a waste sample and test for contaminants.
Similar to a grease interceptor, the holding tank must be placed where it can be easily accessed by a pump truck. Beneath the floor of an ambulance garage is a convenient choice, as the decontamination area is usually nearby. Locating it outdoors near the ambulance entrance is usually the next best choice, but it must then be buried beneath the frost line. Placing it inside the building brings a higher risk of contaminant spread and should be avoided.
• Water heater selection and sizing. Choosing domestic hot water source equipment for decontamination areas can be challenging. If the area is expected to see infrequent use and comprises a small portion of the peak building load, then it is often best to put it on the main domestic hot water system. But if it becomes the main driver of the size of the building water heaters, it is usually more advantageous to give it dedicated equipment.
Tank-type storage water heaters are often a poor choice for this scenario, as they deteriorate more rapidly with infrequent use — decontamination areas rarely see enough demand to overcome this. Instantaneous or semi-instantaneous water heaters are not as susceptible to this; many decontamination areas can be served with a small number of these units, especially if building steam or natural gas is
available.
Like the holding tank, water heaters should be sized to handle all decontamination fixtures running at once for 15 minutes at a minimum. If there is a higher likelihood of mass casualty events, use the total number of patients to be processed in the event, assuming a 15-minute washdown each using the fixture with the highest flow rate.
Water heaters should be set at a temperature that provides Legionella mitigation (140 F is common), but the temperature at the fixture outlets should be no more than 100 F (to avoid scalding) and no less than 80 F (to avoid excessive discomfort and hypothermia).
• Sanitary sewer and vent piping selection. Sanitary sewer and vent piping need to withstand the contaminants that will be passed through it, some of which will be corrosive. Compiling an exhaustive list of these contaminants is usually not practical, so choosing a broad-spectrum material is easier.
Schedule 40 CPVC with solvent cement joints is common, but Schedule 40 or 80 polypropylene with heat-fusion joints is even more robust. Sanitary vent piping should be of the same material, as contaminant vapors can travel through it.
As health care is increasingly pushed to outpatient facilities, expect to see more freestanding emergency departments being built. Decontamination areas are the most plumbing-intensive areas of these projects, and expectations for them vary by client, project location, size and emergency response strategy. When designing these areas, approach each one with a fresh perspective and not based on what was done on a similar prior project.
Aaron Bock, PE, CPD, GPD, LEED AP, EDAC is a senior plumbing engineer at ERDMAN in Madison, Wis., and president of the Wisconsin chapter of the American Society of Plumbing Engineers.


_800x800_webp.webp?t=1775667064)



