Let us do a quick recap since it has been a few months since Part I of this series in the June issue and COVID-19 has blown up. Below are several respiratory therapies which may be implemented regularly:
- Nasal cannula, 8 lpm
- Reservoir masks, 15 lpm
- Standard invasive vent, 12 lpm
- High-flow vents (noninvasive), 50 lpm (COVID-19 patients not likely to use)
- High-frequency oscillating vent, 80 lpm
- CPAP hoods, 50 to 120 lpm
- High-flow nasal cannula, 40 to 60 lpm
We covered what make-ready hospitals look like:
- Arena to Healthcare (A2HC)
- Hotel to Healthcare (H2HC)
- Closed Health-Care Concept (CH2HC)
The resurgence of COVID-19 has drastically increased the use of ventilators and other methods in hospitals over the first part of the summer. It is essential for facility personnel to monitor and understand the capacity of the oxygen and medical air systems to ensure the increased loads can be supported.
Let me first say that there are no one-size-fits-all solutions here. This column will offer a simplified approach to assessing system capacity, including some key areas to monitor as the system demands increase.
As we covered in Part I, the respiratory therapy director should be consulted to understand the potential for other treatment methods and associated equipment; this conversation may need to be ongoing during the evaluation as treatment methods shift. Understanding the likely equipment used is key to planning how a facility’s system will operate under increased consumption and what areas to monitor closely.
A full system assessment should be performed to determine the precise number of ventilators or high-flow nasal cannula that can be supported per zone. This can help guide respiratory therapists and nursing staff to make more informed decisions on where to locate critical patients who require a ventilator or high-flow nasal cannula support/treatment.
The best way to determine how many ventilators or high-flow nasal cannula a facility/system can support starts with a discussion between facility personnel, respiratory therapists, nursing personnel and a medical gas system engineer. Essential information to aid the conversation includes specific ventilators (what the facility uses), as-built or existing conditions drawings for the medical gas system and equipment, and medical gas consumption logs/trends with a typical oxygen delivery schedule.
As a facility identifies the likelihood of increased oxygen consumption, the bulk oxygen supplier will need to be contacted to ensure the demand can be met from a refilling perspective. Many suppliers have increased production to where there is little to no impact.
It’s important to note that these systems are sized per industry recommendations and code requirements. However, the values used in sizing the systems can be different from what is being used in a facility, hence the desire to understand what the installed system can provide and what it might affect if it operates at maximum capacity.
How Many Ventilators?
A stepped, logical process is needed to rationally determine where a facility’s systems have their inherent capacity limitation. Systems will be limited by how quickly they can get oxygen delivered, by the vaporizer capacity, by the main piping risers, by the ventilator capacity for the individual zones, or by the medical air dryers.
Some guiding questions can be addressed to help develop the analysis:
• How many ventilators does the facility have? Which models? What flow rate?
• Which zones are the ideal targets for heavy ventilator use? Critical care and ICU areas? General medical/surgical patient areas? Specialized zones/wards?
• What are typical baselines of oxygen and medical air used by the facility? Analyze some basic trends of oxygen deliveries for various times of the year. Is it significantly elevated during winter months (flu season)? Is there a substantial amount of oxygen and medical air used for elective procedures that will be different during a crisis?
• Under typical conditions, is icing on the vaporizer a problem? If so, how is it typically resolved?
• What is the maximum delivery frequency and size that can be expected from the supplier? Is this going to be further limited by increased demand by other facilities in the area?
• Does the facility have any spares to mitigate concerns of failures? For instance, compressors already stored on-site for quick replacement of the medical air compressor or possibly spare vaporizers or dryers?
Basic Rules of Thumb
The following rules of thumb attempt to align moderate piping pressure losses with typical pipe sizes. Every facility and system is unique. These values presume no other gas consumption is occurring aside except ventilators or high-flow nasal cannula.
In general, it is reasonable to presume the capacities in Table 1 for a zone based on the zone's main pipe size.
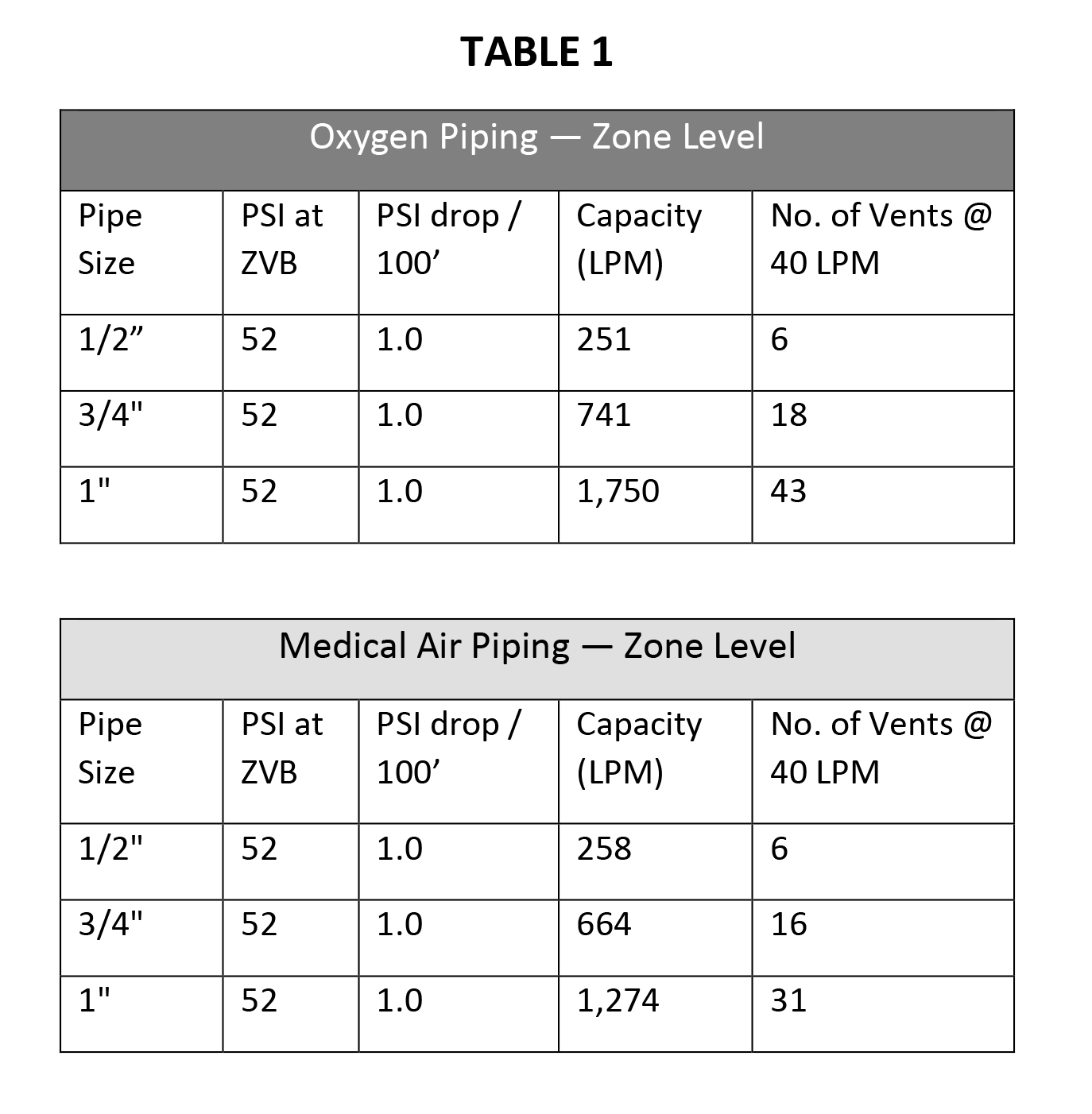
In general, it is reasonable to presume the capacities in Table 2 for system mains and risers based on the zone main pipe size.
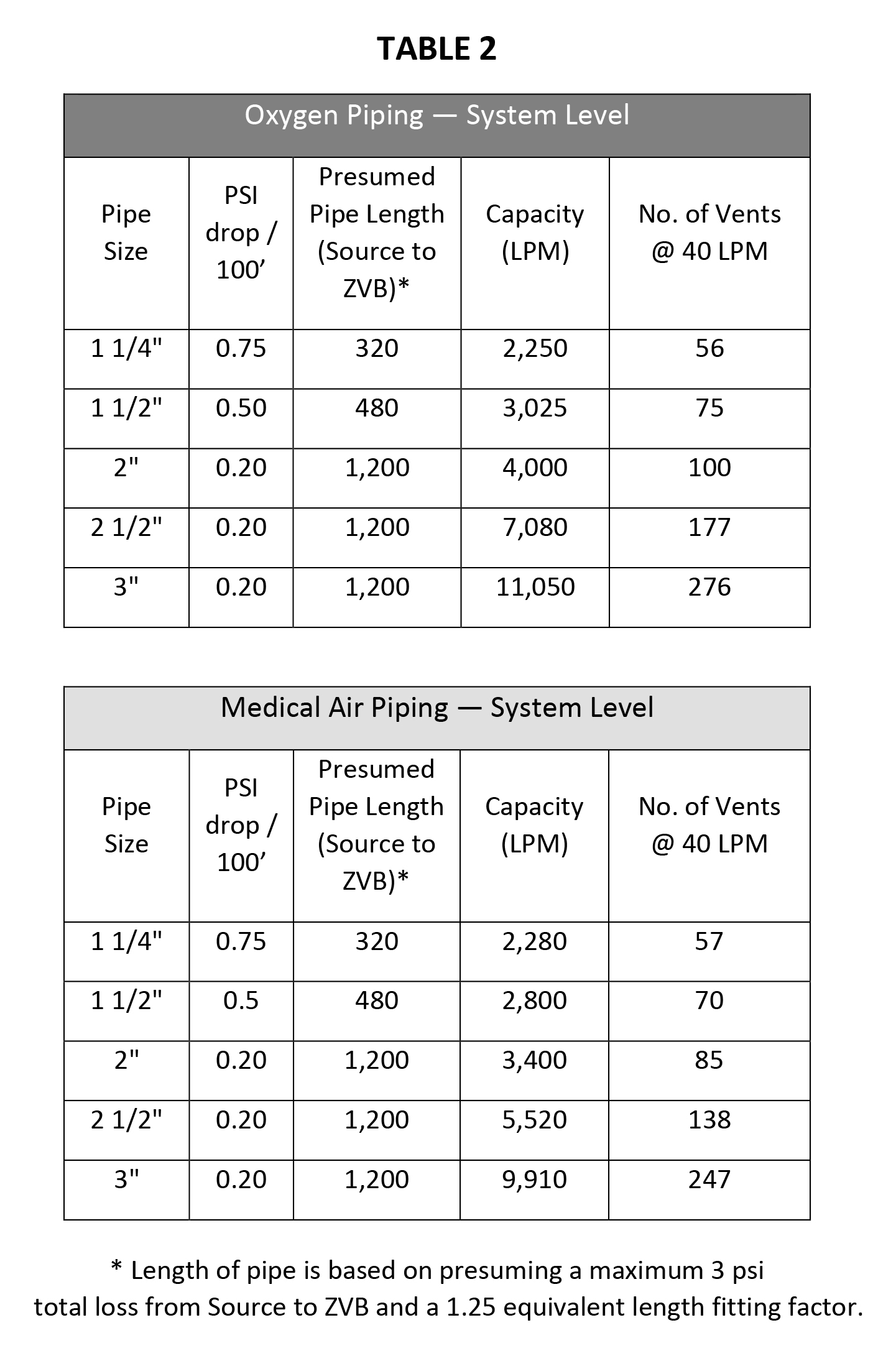
Capacity and Consumption
Keep in mind that while you may have the capacity to support the increased ventilators, will it strain your oxygen vaporizers? Can suppliers deliver oxygen consistent enough to meet your anticipated demand? Will other facilities they service have increased demand as well? Typical delivery vessels can supply 3,500 gallons to 4,000 gallons of liquid oxygen, which is substantial in ventilator and high-flow nasal cannula support.
Ventilators do not continuously flow the rated oxygen and medical air. They emulate a natural breathing rhythm. The system must be able to deliver the capacity required at the connection, but the gasses are not consumed constantly; they only flow during the patient’s intake breath. Given any ventilator flow rate, presuming a 1-second breath duration and that the average breathing rate of a sick patient of 20 breaths per minute — the source consumption is approximately one-third of the ventilator rated flow.
Based on the values shown in Tables 1 and 2, this would equate to an oxygen consumption rate of approximately 13.3 LPM at the bulk source. This value can be used for source analysis to determine the proper capacity of support within the bulk storage tank(s), vaporizer(s) and oxygen delivery capabilities.
Converting the oxygen used by the ventilator at the source level, its use depletes approximately 13.3 LPM (gas), which is approximately 5.9 gallons of liquid oxygen per day (see Table 3).
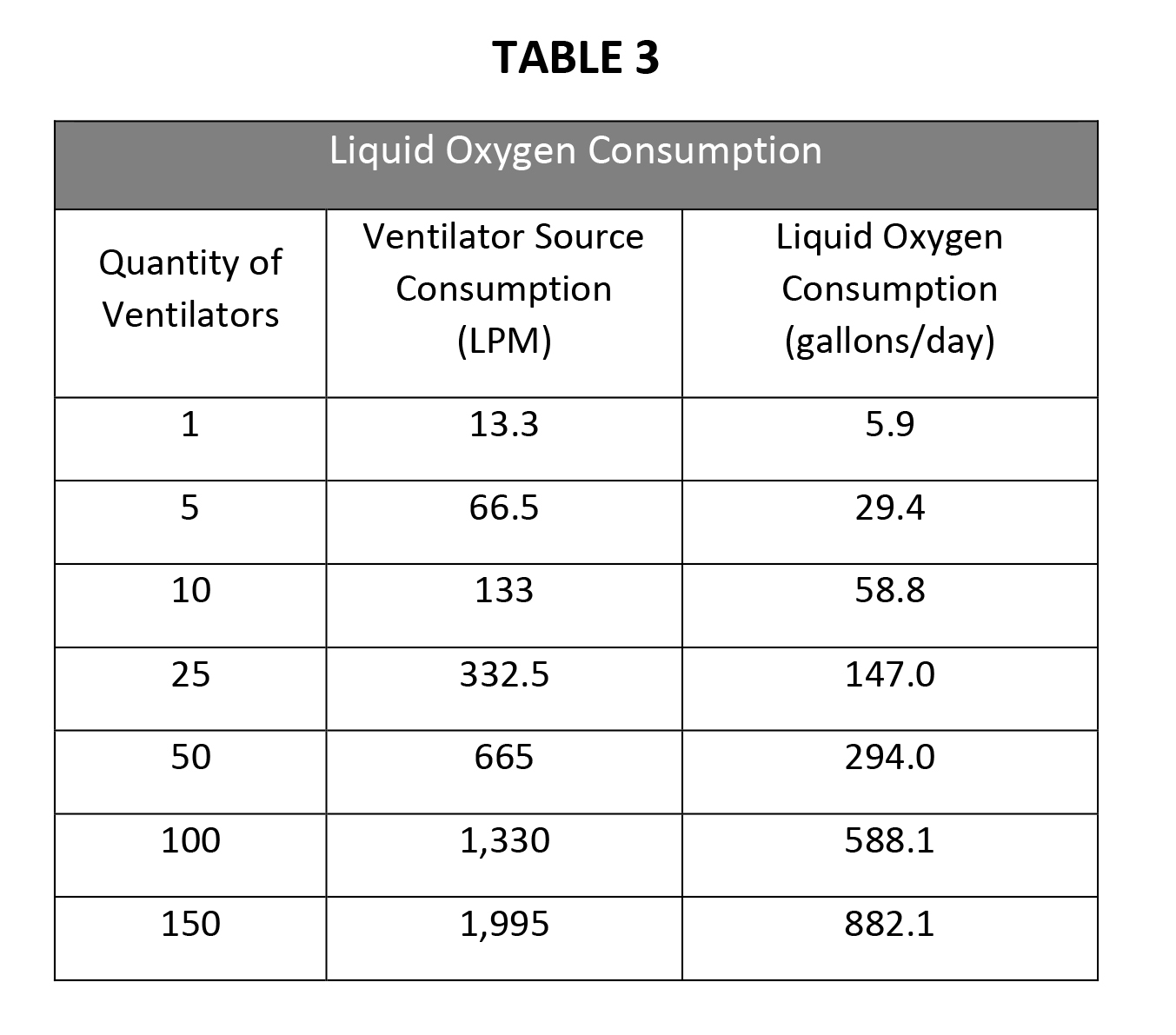
The main discussion has been centered around ventilators because those require a relatively high flow rate for operation and are the most widely used. Another respiratory therapy method gaining popularity is the use of high-flow nasal cannula, which has similar flow rates but are more constant.
The flow through a given pipe size can be increased if the pressure loss associated with that pipe can be increased. High-flow nasal cannula can be used in the same zone as ventilators if the pressure at the zone valve box will be monitored.
Keep an Eye on Things
As your oxygen consumption increases, the vaporizers will run an increasing risk of icing; this is especially problematic in humid climates. Icing will decrease the rate at which oxygen converts from liquid to gas and, thus, can starve your system. Icing could reduce the vaporizer capacity by 50 percent.
Keep an eye on the medical air as well. If the driers cannot keep up with the demand, they will begin to develop moisture in the system, which may have a long-term effect inside the piping system.
A more detailed white paper we developed should suitably arm facility personnel and planners to have a conversation regarding crisis level ventilator management using the systems with minimal or no modifications.
Before a hospital is projected to see a surge in ventilator requirements beyond what has typically been observed during previous flu seasons, a more detailed analysis should be warranted.
If the hospital is planning on concentrating COVID-19 patients to certain areas or expanding areas in support of COVID-19 patients, then a more thorough analysis is warranted to help identify where the existing system capacity can already afford the added consumption.
Just before submitting this column, we came across this article from the American Association for Respiratory Care: “Additional Ventilators May Pose a Risk to Hospital Gas Systems” (https://bit.ly/2DHgue5). It provides a helpful link to estimating gas requirements.

_800x800_webp.webp?t=1775667064)



